Intermittent fasting (IF) to improve blood sugar management and metabolic health?
Can IF improve your blood sugar management? What about metabolic health? If you are at risk of developing type 2 diabetes or currently have it, you may indeed be interested in this.
Table of contents:
- What’s the fuss about IF?
- What does the research show?
- However…
- Proven recommendations to improve and optimise your metabolic health
- Take aways
What’s the fuss about IF?
Animal studies suggest that IF may have inherent benefits, providing superior effects to calorie restriction, such as improving insulin sensitivity and cardiovascular health. Importantly, animal studies indicate that the benefits of IF may take place without weight loss.
However, whether the switch between the fed and fasting state, or at least in the capacity that protocols commonly used do, provide the same benefits in humans remains unclear. The literature on IF in humans is limited and there are numerous confounding factors that limit being able to draw conclusions.
What does the research show?
Whilst there are studies to show that IF may improve blood sugar and fat levels (1,2,3) as well as fasting insulin levels (2,3), weight loss and calorie restriction are independently associated with these improvements. Therefore whether these benefits can be attributed to IF is questionable.
A systematic review of trials lasting over six months reported no difference between IF and continuous caloric restriction for blood sugar, fat and insulin levels (4).
Additionally, a study on alternate day fasting found similar results between IF and continuous caloric restriction, but additionally found IF to have a detrimental effect on LDL (low density lipoprotein) cholesterol levels (5).
In a study where one IF group were calorie restricted and the other were not, the IF group that were not calorie restricted did not experience any improvements in metabolic health (3).
Verdict: evidence is currently lacking to support the idea that IF inherently provide greater improvements in metabolic health than other methods of caloric restriction.
It appears to be the weight loss and fat loss that provide the benefits for metabolic health.
However…
If you are overweight and find IF beneficial for weight loss, then a reduction in weight will definitely be associated with improvements in your metabolic health.
Additionally, if you for IF for weight management and remaining at a healthy weight, then this will be beneficial for your metabolic health.
Proven recommendations to improve and optimise your metabolic health
Lose excess middle region body fat: as this excess middle located body fat, known as visceral fat, is strongly associated with increased risk of chronic disease such as cardiovascular disease and type 2 diabetes (6).
You can be at a “normal BMI” but if you have excess body fat located in the middle region of the body, around the organs, known as visceral fat, then you are at increased risk of developing conditions such as type 2 diabetes (7). In fact, 25% of people who are metabolically unhealthy are not overweight.
If you have excess fat stores then you need to create a calorie deficit to lose these.
Progress towards being a “healthy” weight for you: as you will be less likely to have excess body fat which can become unhealthy. Excess body fat is strongly associated with poor metabolic health because of its pro inflammatory effects.
Again, weight loss is achieved by creating a meaningful calorie deficit.
Exercise regularly: both aerobic exercise and a combination of aerobic and resistance exercise are associated with improved blood pressure, blood fat and cholesterol levels as well as fasting blood sugar levels. Regular exercise is associated with reduced risk of developing chronic disease (8).
Combine aerobic and resistance exercise: whilst we know that aerobic exercise benefits metabolic health, lifting heavy things, aka resistance exercise is great for increasing insulin sensitivity.
More muscle means more disposal for that sugar to move out of your blood stream. Additionally, it will increase your metabolism and reduce your risk of developing chronic disease.
Include components from the Mediterranean diet: since there is strong evidence to indicate that a Mediterranean style diet may benefit individuals who are at risk of developing or who have type 2 diabetes (9,10,11).
A Mediterranean diet may be more beneficial for increasing levels of a substance associated with insulin sensitivity (adiponectin), increasing levels of insulin sensitivity and reducing levels of an inflammatory marker (CRP) (12).
Check out the copied image below for what this may look like – taken from (13).
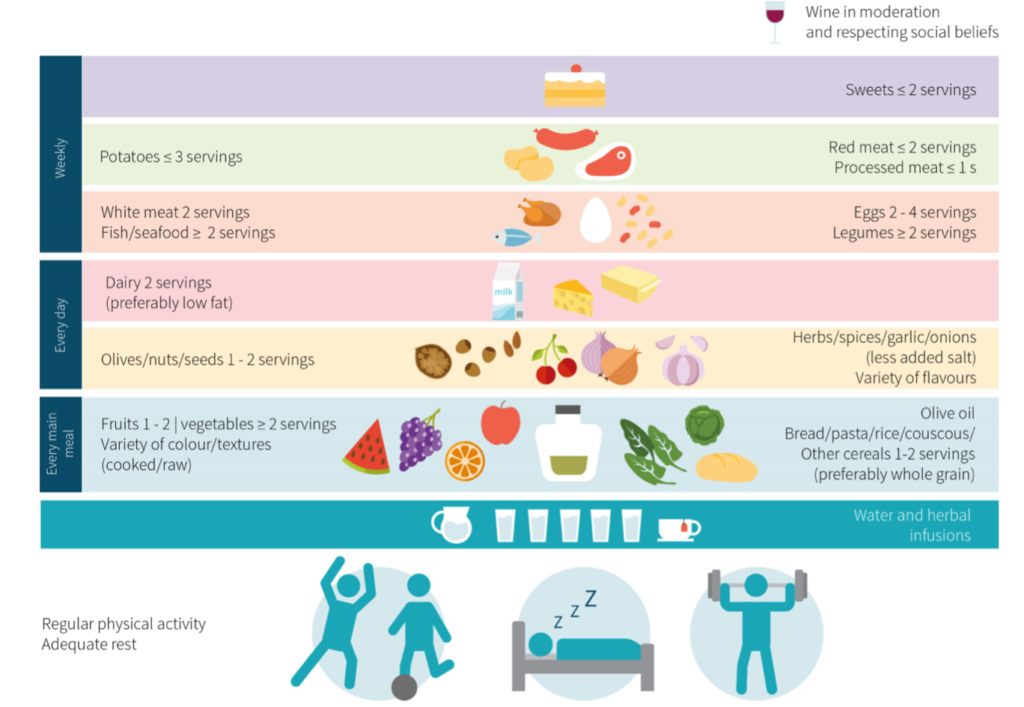
An approximate guideline for macronutrient intakes may be – 30-40% from carbs, 30-40% from fats (saturated fats <10% and focusing on mono and poly unsaturated fats) and 20-30% from protein.
Take aways
Prioritise reducing excess body fat levels: excess body fat is pro inflammatory. If you lose this, you will automatically improve metabolic health. This can be obtained through creating an appropriate calorie deficit – using a personalised nutritional plan that suits your needs and energy requirements.
Consistence adherence to the diet is what matters – so consider whether IF is a tool for you to achieve this.
Include regular exercise: to significantly improve metabolic health – from reducing levels of inflammation, to increasing insulin sensitivity, to increasing energy output.
Create an exercise schedule that you can realistically achieve. Review it after a few weeks. Ideally include a mixture of aerobic and resistance exercise.
Follow a diet that is 80% whole foods and include local produce when possible: as this will help for you to have a nutrient rich diet and likely benefit weight management. Include a couple of non-starchy veg at every meal (e.g. broccoli, cauliflower, kale, swiss chard, Romano peppers) and low sugar fruits such as blueberries and raspberries daily.
Have a minimum 12 hour fasting window: note the time that you finish your last bite of food and don’t have your next meal for another 12 hours. For example, if you finish your last meal at 8pm then don’t have breakfast until after 8am.
If your metabolic health is poor and/or you are overweight, shoot for a 14 hour fasting window if you feel this is achievable.
However, you can build up to this fasting window and prioritise meeting your calorie deficit to lose excess fat over meeting a specific fasting window (this obviously isn’t applicable to athletes).
Related articles
Intermittent fasting for weight loss and body composition?
Fasted cardio for better weight and fat loss??
What are your thoughts on IF for blood sugar management and metabolic health?
References
- Antoni et al. (2018). Intermittent vs continuous energy restriction: differential effects on postprandial glucose and lipid metabolism following matched weight loss in overweight/obese participants.
- Harvie et al. (2011). The effects of intermittent or continuous energy restriction on weight loss and metabolic disease risk markers: a randomised trial in young overweight women.
- Hutchinson et al. (2019). Effects of intermittent versus continuous energy intake on insulin sensitivity and metabolic risk in overweight women.
- Headland et al. (2016). Weight-loss outcomes: a systematic review and meta-analysis of intermittent energy restriction trials lasting a minimum of 6 months.
- Trepanowski et al. (2017). Effect of alternate-day fasting on weight loss, weight maintenance, and cardioprotection among metabolically healthy obese adults: a randomised clinical trial.
- Ross et al. (2020). Waist circumference as a vital sign in clinical practice: a consensus statement from the IAS and ICCR working group on visceral obesity.
- Zhu et al. (2002). Waist circumference and obesity-associated risk factors among whites in the third National Health and Nutrition Examination Survey: clinical actions thresholds.
- Ostman et al. (2017). The effect of exercise training on clinical outcomes in patients with the metabolic syndrome: a systematic review and meta-analysis.
- Esposito et al. (2015). A journey into the Mediterranean diet and type 2 diabetes: a systematic review and meta-analysis.
- Esposito et al. (2009). Adherence to the Mediterranean diet and glycaemic control in Type 2 diabetes mellitus.
- Elhayanya et al. (2010). A low carbohydrate Mediterranean diet improves cardiovascular risk factors and diabetes control among overweight patients with type 2 diabetes mellitus: a 1-year prospective randomised intervention study.
- Maiorino et al. (2016). Mediterranean diet cools down the inflammatory milieu in type 2 diabetes: the MEDITA randomised controlled trial.
- Bach-Faig et al. (2011). Mediterranean diet pyramid today. Science and cultural updates.

Leave a Reply Cancel reply
Subscribe to my monthly newsletter
Site Credit
LEGAL
FAQS
CONTACT
© 2023 Antonia Osborne
Antonia,
MSc, RNutr
Performance Coach
Registered Sports & Exercise Nutritionist
Interesting, I’ve heard of successful management of diabetes with intermittent fasting.
Hannah,
I think the successful management is likely due to either:
– the weight loss
– the weight management
– eating within a time of day that is preferential for blood sugar management